At a glance
1.5 days
High-fidelity prototype
6 weeks
To first release
6+ CCGs
Onboarded in week one
48 hours
Deployment guarantee
Client: my mhealth, a class 1 MHRA-regulated medical device manufacturer. Role: Chief Product Officer, leading design and user research end to end. Live in NHS wards from 1st May 2020. The platform went on to win the Judges' Choice for Excellence in Digital Health Innovation at the Juniper Research Future Digital Awards 2021, recognised alongside Teladoc and Google.
The problem
In March 2020, the UK was weeks into its first national lockdown. The NHS Confederation warned that a 30% drop in 2020 treatment referrals could produce a six-million patient backlog. Clinical teams needed a way to monitor at-risk patients with suspected or confirmed COVID-19 remotely, reducing demand on hospital services while safely managing deterioration at scale.
There was no time for a conventional product development cycle. The product had to be clinically safe, MHRA-compliant, usable by patients ranging from digital natives to care home residents, and deployed into live NHS wards within weeks.
My role
As Chief Product Officer at my mhealth, I led design and user research for the COVID-19 Virtual Ward end to end. Both the patient-facing app and the clinician web tool. I worked directly with the dev team, clinical lead, and CEO from day one, and with NHS clinical teams throughout to iterate on the product in the hands of real users.
Approach
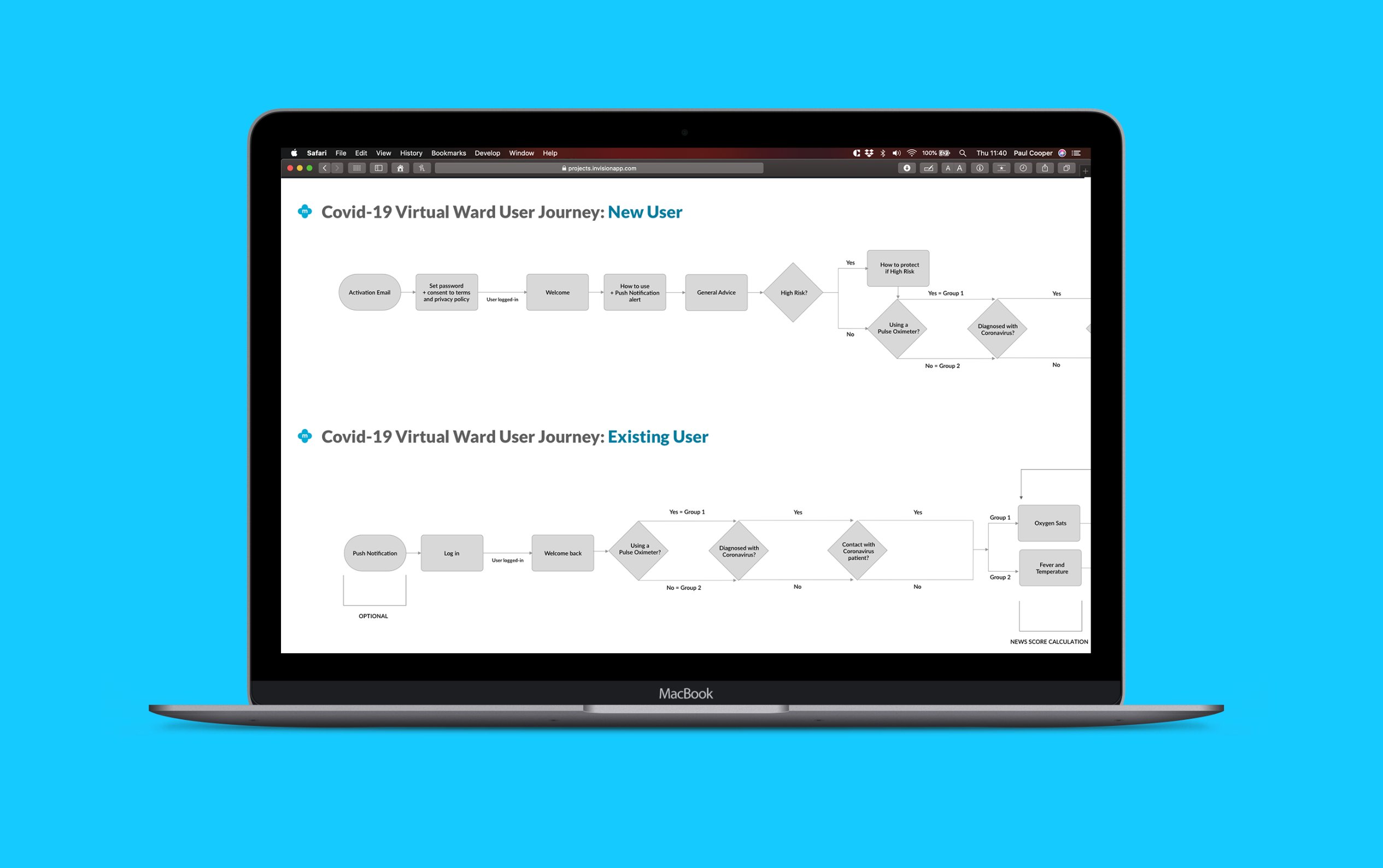
Accelerated design process. A single kick-off meeting with the dev team, clinical lead, and CEO to pin down the problem. I produced a full high-fidelity prototype in 1.5 days, using my mhealth's existing Sketch design system and Invision to keep fidelity high without starting from scratch. Design decisions were deliberately constrained to what could be shipped, tested, and improved in-flight rather than perfected up front.
Two products, one system. A patient-facing app (symptoms, pulse oximeter readings, NHS England Remote Monitoring Guidelines-aligned alerts) and a clinician web tool (patient list, NEWS score triage, notifications). Consistent visual and interaction patterns across both to reduce training overhead for NHS teams deploying under pressure.
Design decisions that mattered.
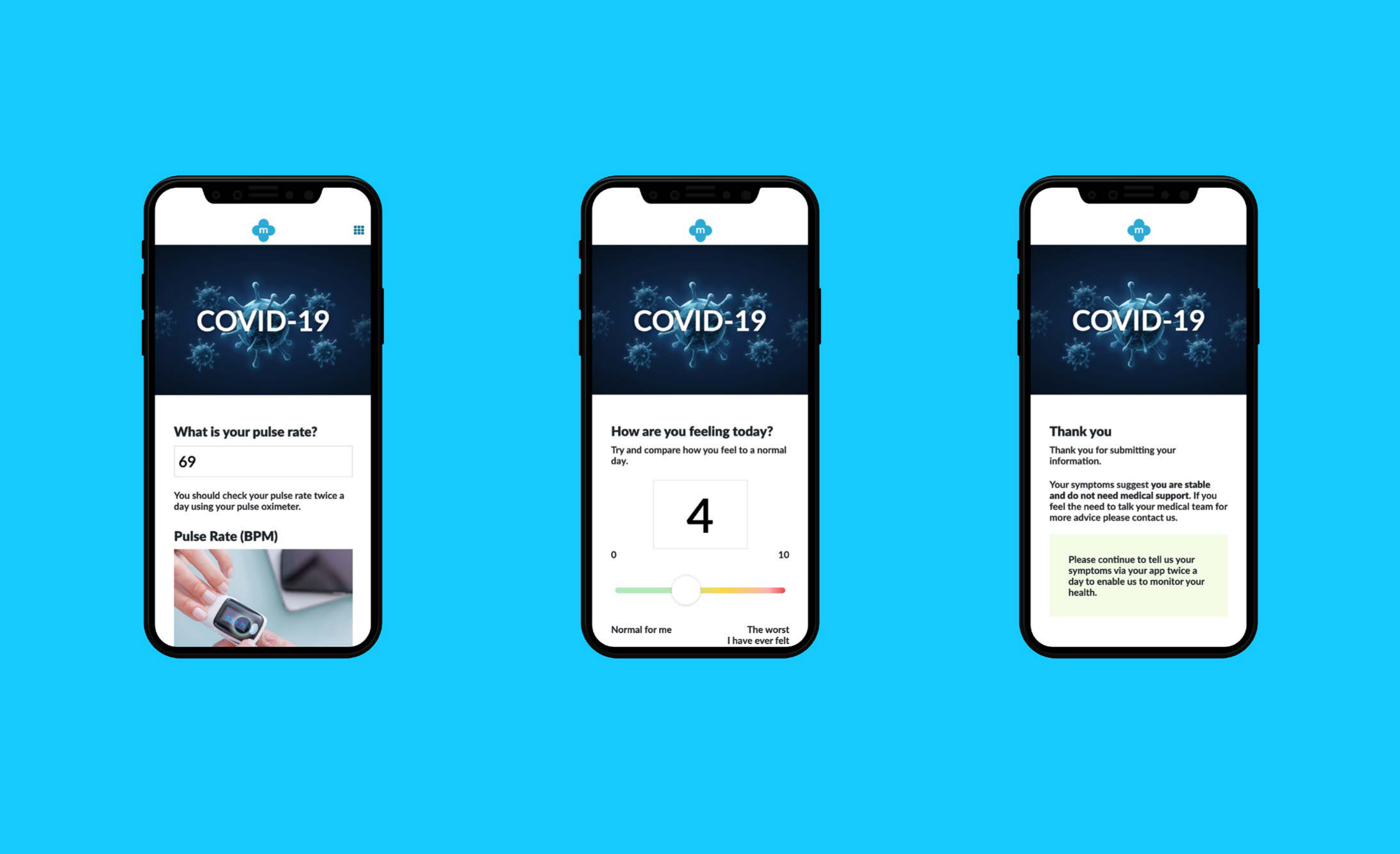
- gov.uk design principles as the foundation. Accessible, consistent, designed with data. Patients ranged from digitally confident users to elderly care home residents, and the product had to work for both on the first attempt.
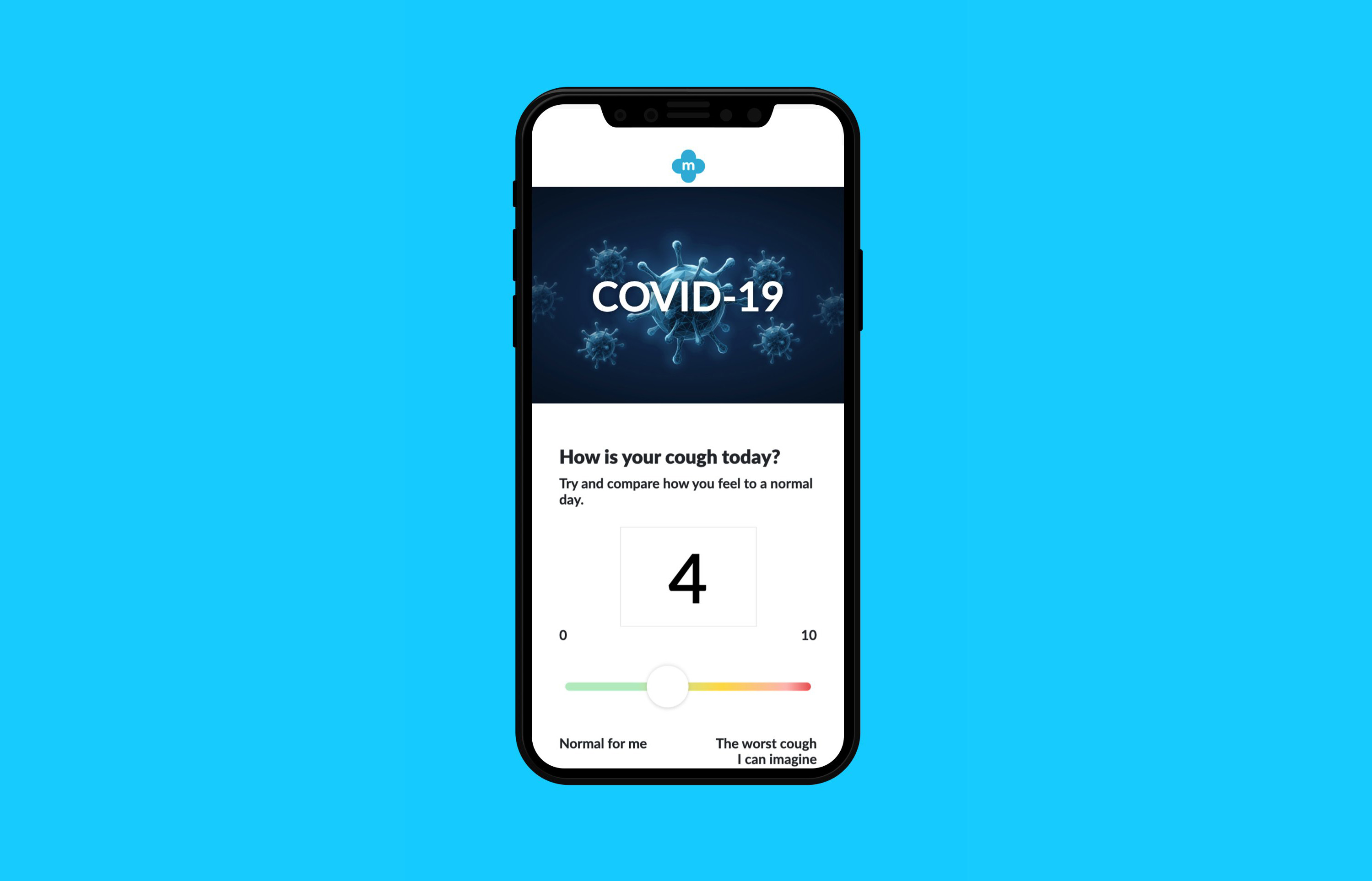
- Virus imagery used deliberately on the symptom-entry screen. Familiar from media coverage, it conveyed urgency and helped patients understand why accurate daily input mattered.
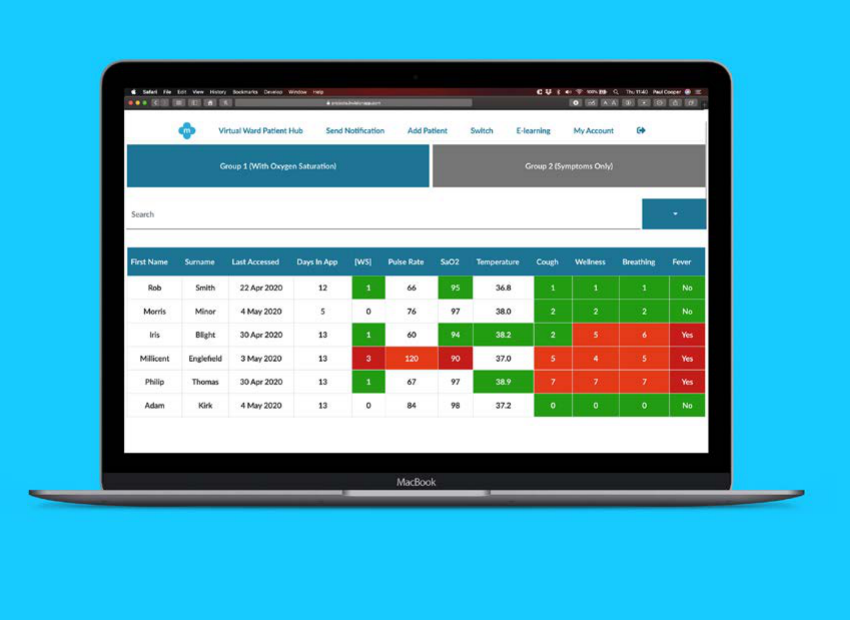
- NEWS score calculation built into the clinician view with clear colour-coded thresholds so clinical teams could triage at a glance across a growing patient list.
Research in-flight. With no time for a prototype-first research cycle, user research ran on the live beta. Clinicians at the Tees Valley NHS Vanguard Unit (Hartlepool & Stockton Health GP Federation) used the app over a weekend with dummy patient data. Their feedback fed directly into the alpha, which was tested with a small patient cohort in the New Forest before national rollout.
Iterations that came from real use
Two improvements from live clinical feedback that meaningfully changed the product:
Clinician-entered patient data. During alpha testing with care home nurses, we discovered some patients could not use the app themselves. No smartphone, no computer, or too unwell. The solution was a new clinician-side function to register and input data on behalf of patients. This unlocked deployment into care home settings that would otherwise have been excluded.
Patient list triage affordances. In-depth user research with nurses at H&SH revealed they were phoning patients to take symptoms verbally, then entering data themselves from long patient lists. I added a visual indicator for this patient type and a checkbox to mark results as assessed. Small change, meaningful impact on nurse workload.
What shipped
- Patient-facing app (web, iOS, Android) with symptom tracking, pulse oximeter input, and automated alerts aligned to NHS England COVID-19 Remote Monitoring Guidelines.
- Clinician web tool with patient list, NEWS score triage, group management, and notifications.
- MHRA-compliant design documentation supporting class 1 medical device status.
- A 48-hour deployment playbook that took the product from signed contract to active ward in two days.
- Sketch
- Invision
- NHS design system
- gov.uk principles
- MHRA class 1
Outcomes
The app went live with first patients on 1st May 2020. Within the first week of release, 6+ CCGs had begun onboarding patients. By August 2020, it had matured into a productised offering available through the CCS Spark DPS framework, with a guaranteed 48-hour deployment for any NHS trust that signed a contract.
The COVID-19 Virtual Ward app is really straightforward to use. By working directly with my mhealth to make changes based on our clinician's experience when testing the app, we've been able to work more efficiently and help more patients during the COVID-19 pandemic.
In 2021, my mhealth's wider digital therapeutics platform won the Judges' Choice for Excellence in Digital Health Innovation at the Juniper Research Future Digital Awards.